700 Glenhuntly Road
Caulfield VIC 3162
03 9044 4555

700 Glenhuntly Road
Caulfield VIC 3162
03 9044 4555
Knee Arthroscopy
Knee Arthroscopy
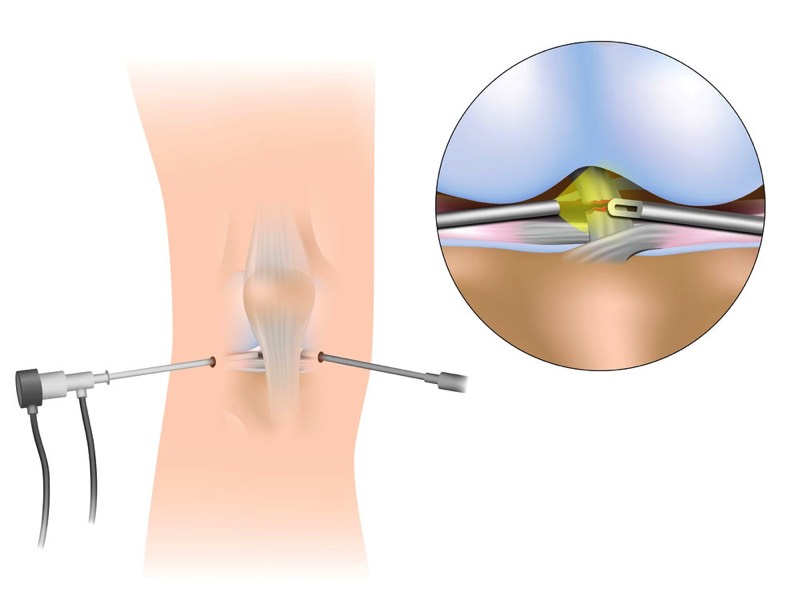
Knee arthroscopy is surgery done using key-hole (1cm long) incisions and a telescope (“arthroscope”) inserted into the knee joint. A number of different knee conditions can be treated using arthroscopic surgery.
These include:
Arthroscopic surgery is frequently done under a general anaesthetic. Once under ansaesthetic and the leg has been prepared, two or three keyhole incisions are made at the front of the knee, on either side of the patella tendon. Next a 4mm diameter arthroscope is introduced into the knee to survey the various cartilage surfaces of the femur, patella and tibia, as well as the menisci and the anterior and posterior cruciate ligaments. The integrity of these structures can be seen and they can be tested to see if they’ve been damaged with the use of a small probe. The medial and lateral collateral ligaments cannot usually be seen directly as they lie outside the knee joint itself. If any damaged material is seen within the knee, then small tools and sutures can be introduced into the knee to remove or repair the damaged tissues.
The operative time of an arthroscopy can vary enormously, depending on what needs to be done within the knee. The majority of procedures usually only require a day-stay in hospital, being discharged home later on the same day. You will usually be able to walk on the same day with the use of crutches.
The benefits of arthroscopic knee surgery, in general, is less trauma to the tissues surrounding the knee and so there is usually a shorter rehabilitation. Despite these small skin incisions, fairly involved and extensive surgery can be performed inside the knee and so there may be more discomfort or swelling than might be otherwise expected, with relatively little outward sign of what has been done inside the knee joint.
A torn meniscus is one of the most common reasons for having a knee arthroscopy, which aims to alleviate the symptoms related to the meniscal tear. These may include localised pain, swelling, catching, clicking and locking of the knee. Depending on the age of the patient, the type of injury and location of the tear within the meniscus it may be feasible to repair the torn meniscus arthroscopically. The concept of meniscal preservation where possible is important to maintain the function of the meniscus for as long as possible. If mensical repair is not possible, then the damaged portions of the meniscus may be removed instead.
Sometimes when there is early arthritis within a knee joint, there may be associated cartilage tears or flaps, which cause similar symptoms to meniscal tears. These cartilage flaps are not repairable, and are usually part of the arthritic process inside the knee. Nevertheless, debriding the flap to a smooth and stable base can alleviate symptoms previously described. The recovery from these mechanical symptoms could be expected to be similar to removing a torn meniscus, however, arthritic symptoms such as aching and swelling may remain or even deteriorate despite having removed the local mechanical problem.
Knee arthroscopy is generally considered a very safe procedure which is well tolerated, however like any surgery there is the potential for complications. These can be classified as general complications and those specific to this operation.
These complications relate to all types of orthopaedic surgery and include those related to the anaesthetic, wound site infection, bleeding and damage to nerves and blood vessels. Lower limb orthopaedic surgery also carries the risk of deep venous thrombosis and pulmonary embolism (DVT and PE). Please refer to the General Orthopaedic Surgical Complications information sheet for further details of these complications. Regarding knee arthroscopy in particular, there is the potential for ongoing pain to persist.
Stiffness and Swelling
This is usually fairly transient and self-limiting. During an arthroscopy, the knee is irrigated with sterile fluid to allow for better visualisation of the joint. The soft tissue within the knee often swell which can lead to stiffness, particularly if physiotherapy is not performed postoperatively.
Recurrent injury and meniscal tear
If there has been treatment to a torn meniscus, it is possible to re-tear a repaired meniscus or to have a new tear in a previously damage meniscus that has been debrided. Adhering to post operative instructions and plans from your surgeon and physiotherapist should minimise this risk. If a re-tear or new tear does occur, then further surgery may be required.
These include:
- Removal of part of, or repair of a damaged meniscus
- Removal of loose bodies within the knee joint
- Removal of loose, unstable flaps of degenerative/arthritic cartilage
- As part of reconstructive surgery to treat a torn anterior or posterior cruciate ligaments
- As part of a procedure that can be used to stabilise dislocating patellae
- Removal or biopsy of inflamed synovium from inside the knee joint
- Occasionally as a means of diagnosing and treating infection within the natural knee joint.
Arthroscopic surgery is frequently done under a general anaesthetic. Once under ansaesthetic and the leg has been prepared, two or three keyhole incisions are made at the front of the knee, on either side of the patella tendon. Next a 4mm diameter arthroscope is introduced into the knee to survey the various cartilage surfaces of the femur, patella and tibia, as well as the menisci and the anterior and posterior cruciate ligaments. The integrity of these structures can be seen and they can be tested to see if they’ve been damaged with the use of a small probe. The medial and lateral collateral ligaments cannot usually be seen directly as they lie outside the knee joint itself. If any damaged material is seen within the knee, then small tools and sutures can be introduced into the knee to remove or repair the damaged tissues.
The operative time of an arthroscopy can vary enormously, depending on what needs to be done within the knee. The majority of procedures usually only require a day-stay in hospital, being discharged home later on the same day. You will usually be able to walk on the same day with the use of crutches.
The benefits of arthroscopic knee surgery, in general, is less trauma to the tissues surrounding the knee and so there is usually a shorter rehabilitation. Despite these small skin incisions, fairly involved and extensive surgery can be performed inside the knee and so there may be more discomfort or swelling than might be otherwise expected, with relatively little outward sign of what has been done inside the knee joint.
A torn meniscus is one of the most common reasons for having a knee arthroscopy, which aims to alleviate the symptoms related to the meniscal tear. These may include localised pain, swelling, catching, clicking and locking of the knee. Depending on the age of the patient, the type of injury and location of the tear within the meniscus it may be feasible to repair the torn meniscus arthroscopically. The concept of meniscal preservation where possible is important to maintain the function of the meniscus for as long as possible. If mensical repair is not possible, then the damaged portions of the meniscus may be removed instead.
Sometimes when there is early arthritis within a knee joint, there may be associated cartilage tears or flaps, which cause similar symptoms to meniscal tears. These cartilage flaps are not repairable, and are usually part of the arthritic process inside the knee. Nevertheless, debriding the flap to a smooth and stable base can alleviate symptoms previously described. The recovery from these mechanical symptoms could be expected to be similar to removing a torn meniscus, however, arthritic symptoms such as aching and swelling may remain or even deteriorate despite having removed the local mechanical problem.
Potential Complications
Knee arthroscopy is generally considered a very safe procedure which is well tolerated, however like any surgery there is the potential for complications. These can be classified as general complications and those specific to this operation.
General complications
These complications relate to all types of orthopaedic surgery and include those related to the anaesthetic, wound site infection, bleeding and damage to nerves and blood vessels. Lower limb orthopaedic surgery also carries the risk of deep venous thrombosis and pulmonary embolism (DVT and PE). Please refer to the General Orthopaedic Surgical Complications information sheet for further details of these complications. Regarding knee arthroscopy in particular, there is the potential for ongoing pain to persist.
Specific Complications for Knee Arthroscopic Surgery
Stiffness and Swelling
This is usually fairly transient and self-limiting. During an arthroscopy, the knee is irrigated with sterile fluid to allow for better visualisation of the joint. The soft tissue within the knee often swell which can lead to stiffness, particularly if physiotherapy is not performed postoperatively.
Recurrent injury and meniscal tear
If there has been treatment to a torn meniscus, it is possible to re-tear a repaired meniscus or to have a new tear in a previously damage meniscus that has been debrided. Adhering to post operative instructions and plans from your surgeon and physiotherapist should minimise this risk. If a re-tear or new tear does occur, then further surgery may be required.
The information above is general. All surgical procedures involve some risk. If you would like advice on your specific condition, please contact Oasis Orthopaedics to make an appointment with one of our specialists.